The Swedish Palliative Care Guide (S-PCG)
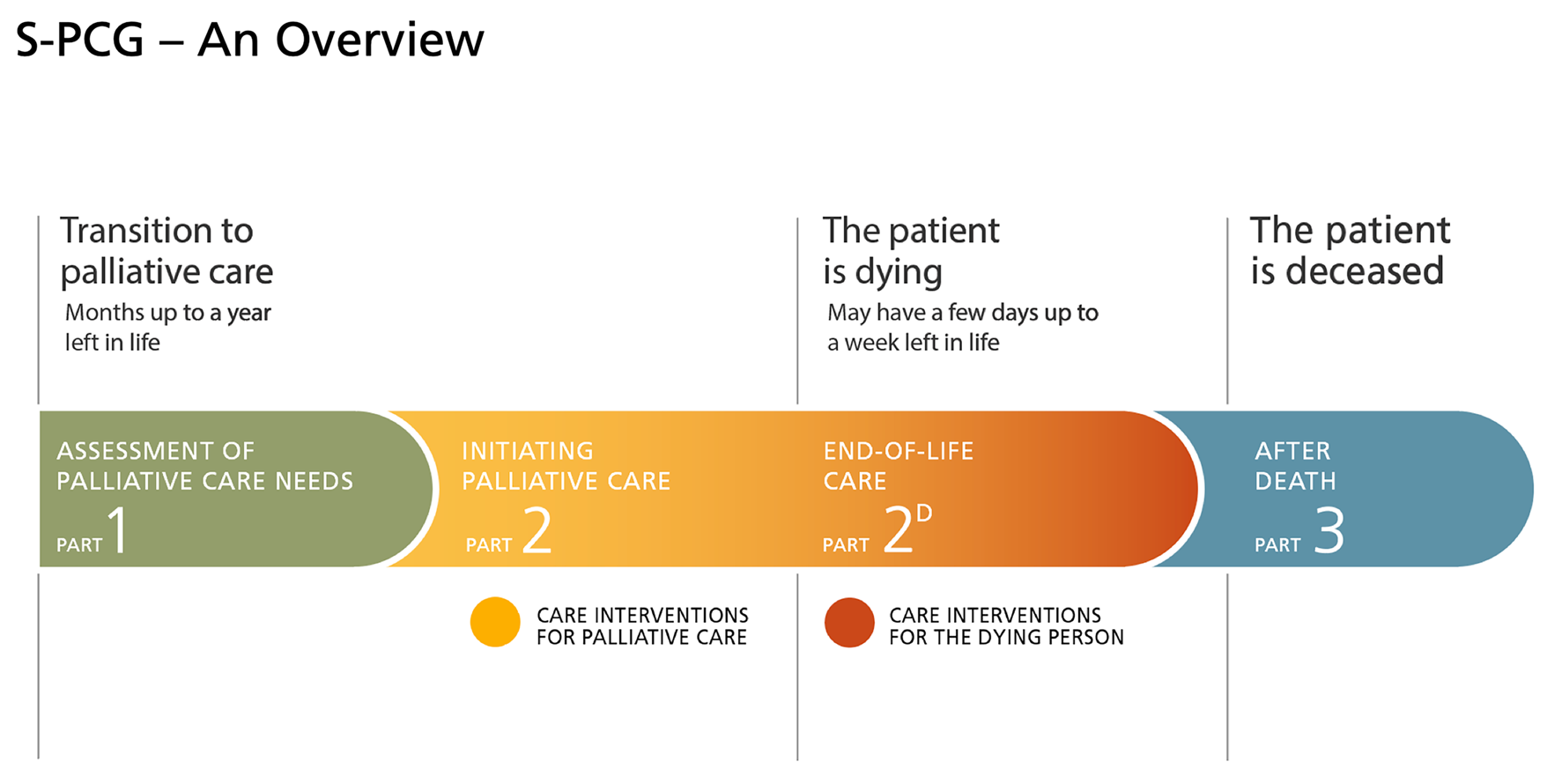
The Swedish Palliative Care Guide (S-PCG) was designed to give support and structure to the interdisciplinary health care team when meeting adult patients with potential palliative care needs. Irrespective of diagnosis and place of care. The S-PCG includes three parts that can each be used to identify and assess individual care needs during the whole palliative care trajectory. From early identification to end-of-life care and care after the death, including bereavement care for family members. The S-PCG can be initiated at any stage of the palliative trajectory by choosing the part that is best suited to meet the current needs of the patient. It provides a structure to identify the patients’ status and needs through assessing symptoms, function, social situation as well as to highlight the importance of the patients’ priorities and wishes. By capturing the individual care-needs, the S-PCG can help create an overview and shared understanding of the needs and possibilities beneficial for each patient’s quality of life and for the next of kin. Furthermore, the S-PCG gives a structure to address the needs through personalized care interventions.
The aim is to enhance the quality of care for people with palliative care needs; to optimize wellbeing and dignity, regardless of diagnosis, place of care or time left in life. To give the opportunity to prioritize and communicate what is important and meaningful for those facing serious illness or end of life.
Currently all documents in S-PCG are being translated to English, and will soon be available.
S-PCG Part 1
Part 1 is a two-page concise tool that provides simplified support for the identification of the patients’ palliative care needs and initiate care planning. It can be used wherever patients that might have palliative care needs are encountered, for example in general practice and in- and outpatient hospital care. It can also be used during consultations or as an assessment tool for multi-professional team rounds.
S-PCG Part 2
Part 2 is intended to support the provision of care for patients with palliative care needs regardless of time left in life. Part 2 consists of a guideline for initiating palliative care, assessment tools, and an associated care plan for recommended interventions for common symptoms and problems, which can be individually initiated according to the identified care needs of the patient. It focuses on defining common goals for care, and may support decisions and palliative care in the time range of months or up to a year left in life. Part 2 also has an appendix regarding children as next of kin.
Read S-PCG Part 2 here
S-PCG Part 2D
Part 2D can be initiated when a patient is assessed as likely dying. Part 2D adds on to Part 2, but focuses on the issues and symptoms that are frequent in the last few days of life. It includes guidance to recognize the dying phase in and hence initiate discussions on shifting the goals of care in the awareness of a most likely soon approaching death. Dying patients require frequent attention and symptom assessment, which is now thoroughly supported, including frequent reassessment in the care plan of Part 2D.
S-PCG Part 3
Part 3 comprises a clear and condensed guide and thorough plan for care after death, in accordance with Swedish national care standards. It supports relevant routines after a patient has died, including recommendations on how to care for the deceased person and promotes bereavement support for the family, including children in the family.
Articles
Birgisdóttir D, Duarte A, Dahlman A, Sallerfors B, Rasmussen BH, Fürst CJ. A novel care guide for personalised palliative care – a national initiative for improved quality of care. BMC Palliat Care. 2021 Nov 11;20(1):176. doi: 10.1186/s12904-021-00874-4. PMID: 34763677; PMCID: PMC8582140. Link to the article
Birgisdóttir, D. (2022). LOSING A PARENT TO CANCER AS A TEENAGER – Family cohesion, grief, long-term health and wellbeing and the development of a comprehensive care guide for personalized palliative care. [Doctoral Thesis (compilation), Department of Health Sciences]. Lund University, Faculty of Medicine. Link to the doctoral thesis
Schelin MEC, Fürst CJ, Rasmussen BH, Hedman C (2023) Increased patient satisfaction by integration of palliative care into geriatrics—A prospective cohort study. PLoS ONE 18(6): e0287550. https://doi.org/10.1371/journal.pone.0287550
Link to the article